Meloxicam Price: Generic Options, Dosing Pearls, and the Pain–Mood Link
Answer in a nutshell: Generic meloxicam is usually inexpensive; use the lowest effective dose and screen for GI/renal risk. Combine medication with function-focused strategies.
Introduction
Meloxicam is one of the most widely prescribed nonsteroidal anti-inflammatory drugs (NSAIDs) for arthritis, back pain, and musculoskeletal injuries. Its once-daily dosing and long duration of action make it a convenient choice for patients who need steady relief without multiple pills per day. Just as important, generic meloxicam is inexpensive, often costing only a few dollars a month, which keeps it accessible for chronic conditions where ongoing therapy is needed. Affordability, however, doesn’t make it risk-free. Like all NSAIDs, meloxicam can stress the stomach, kidneys, and cardiovascular system if used carelessly or in the wrong context. Optimal benefit comes from using the lowest effective dose, reviewing interactions, and pairing medication with functional, movement-based recovery strategies.
This article breaks down what drives meloxicam’s price, how to use it safely, and why addressing both pain and mood together yields the best outcomes, ensuring relief doesn’t come at the expense of long-term health or mobility.
Formulations, Typical Doses, and Price Levers
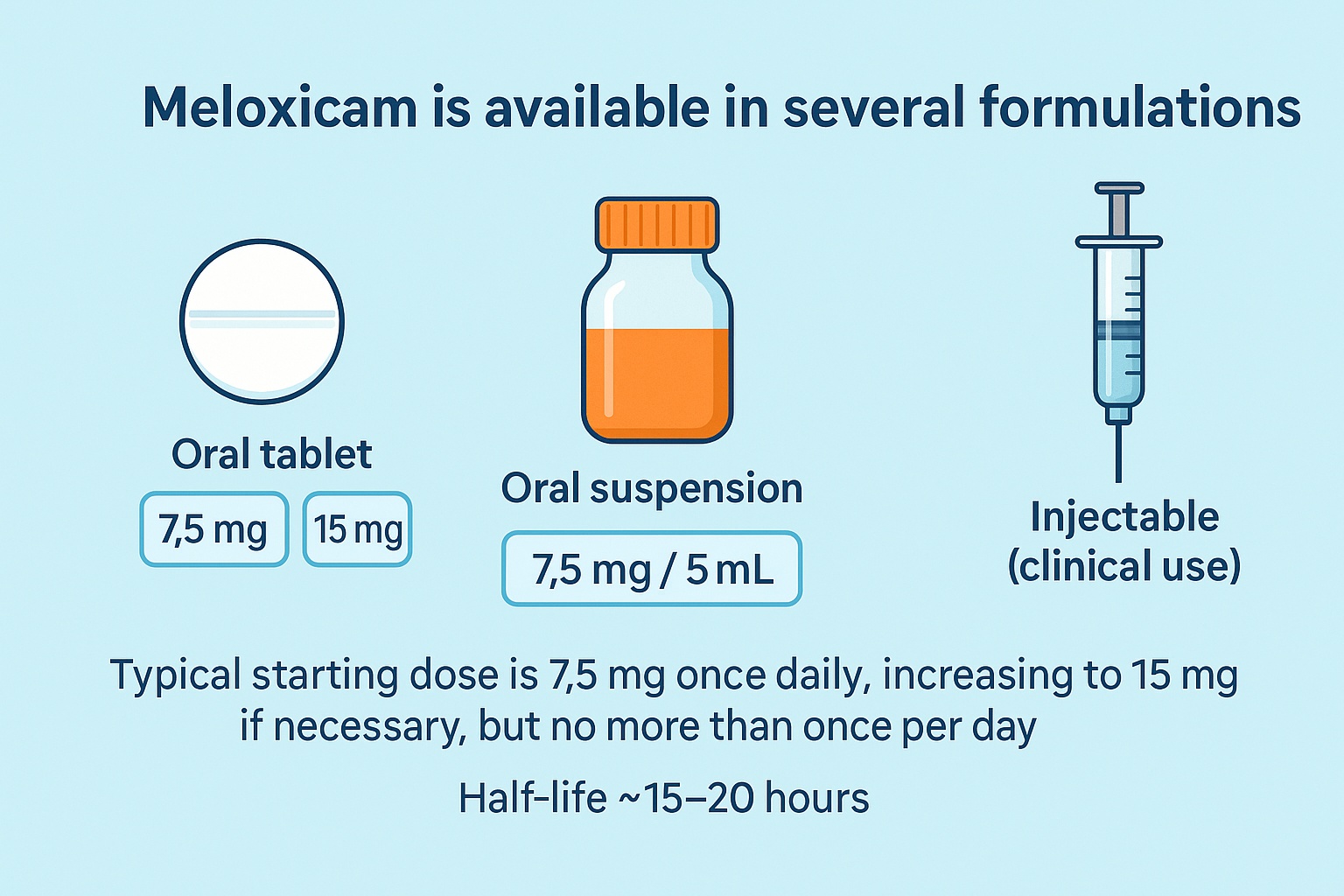 Meloxicam is available in several formulations, most commonly as oral tablets (7.5 mg and 15 mg), but also as oral suspension (7.5 mg/5 mL) and occasionally as an injectable used in clinical settings. For most adults with osteoarthritis or musculoskeletal pain, the typical starting dose is 7.5 mg once daily, increasing to 15 mg if necessary. Because the drug’s half-life is long, roughly 15–20 hours, it provides steady 24-hour relief and should not be taken more than once per day.
Meloxicam is available in several formulations, most commonly as oral tablets (7.5 mg and 15 mg), but also as oral suspension (7.5 mg/5 mL) and occasionally as an injectable used in clinical settings. For most adults with osteoarthritis or musculoskeletal pain, the typical starting dose is 7.5 mg once daily, increasing to 15 mg if necessary. Because the drug’s half-life is long, roughly 15–20 hours, it provides steady 24-hour relief and should not be taken more than once per day.
When comparing prices, meloxicam remains one of the most affordable prescription NSAIDs in the U.S. The generic form usually costs between $0.10 and $0.40 per tablet, depending on strength and pharmacy. A 30-day supply often ranges from $5 to $15 using major discount programs such as GoodRx, Blink Health, or SingleCare. The branded version, Mobic®, rarely offers extra clinical benefit but can cost several times more.
Price levers include:
- Dose size: 15 mg tablets may cost only slightly more than 7.5 mg, so splitting them (if scored and approved by a pharmacist) can cut the per-dose price in half.
- Insurance tiering: many plans list meloxicam as a Tier 1 generic, meaning the lowest copay category.
- Pharmacy type: independent and online mail-order pharmacies often offer the lowest per-month cost.
- Formulation: tablets are cheapest; liquid suspension and brand-name Mobic can be 3–5× more expensive.
To ensure cost transparency, ask for the cash price before filling, even if you plan to use insurance. Sometimes, the uninsured price with a coupon is cheaper than the copay. Although meloxicam’s affordability makes it appealing for long-term use, it should be treated with the same respect as any potent anti-inflammatory. Overuse or combining it with other NSAIDs (ibuprofen, naproxen) doesn’t enhance effect but increases risk. The goal isn’t to take more, it’s to take it strategically, with clear endpoints and safety in mind.
Safety Essentials & Interactions
Although meloxicam is widely used and generally well tolerated, it remains a potent NSAID with real systemic effects. Its benefits depend on dosing precision and awareness of its limits. Meloxicam works by blocking cyclooxygenase (COX) enzymes, which reduces prostaglandin production — the chemical messengers that trigger inflammation, swelling, and pain. Yet prostaglandins also protect the stomach lining and support kidney blood flow, so suppressing them too aggressively can cause problems.
The two most important safety concerns are gastrointestinal (GI) and renal risk. Long-term or high-dose use increases the chance of ulcers, bleeding, and stomach pain, especially in adults over 60 or in those who also take corticosteroids, anticoagulants, or consume alcohol frequently. Taking meloxicam with food or milk reduces irritation, though it does not eliminate the risk entirely. Kidney effects arise when prostaglandin inhibition reduces blood flow through the renal system. People with chronic kidney disease, dehydration, heart failure, or those taking ACE inhibitors or diuretics are especially vulnerable. For these patients, baseline creatinine and eGFR testing is recommended before and during therapy.
Drug interactions deserve equal attention. Combining meloxicam with SSRIs or SNRIs (such as sertraline, fluoxetine, or venlafaxine) or with blood thinners (warfarin, apixaban) raises the risk of GI bleeding. Pairing it with other NSAIDs or regular aspirin compounds toxicity without improving pain control. Similarly, concurrent use with high-dose corticosteroids increases the chance of ulceration.
The safest practice is to use the lowest effective dose for the shortest necessary time. Discontinue the drug if you notice new abdominal pain, black stools, unusual swelling, shortness of breath, or fatigue – all potential early warning signs of adverse reactions.
For those requiring chronic therapy, periodic liver and kidney monitoring helps maintain safety, and gastroprotective strategies (like proton-pump inhibitors) can be discussed with a clinician.
Meloxicam’s selectivity for COX-2 makes it somewhat gentler on the stomach than older NSAIDs, but “gentler” doesn’t mean “risk-free.” Responsible use hinges on informed vigilance, balancing symptom relief with long-term organ protection.
Pain–Mood Spiral and Activity Pacing (Keeping Function on Budget)
Pain and mood are tightly interwoven. Persistent pain doesn’t just strain joints — it reshapes behavior and outlook. The longer discomfort lasts, the more likely it is to erode motivation, social activity, and sleep. Over time, this produces what clinicians call the pain–mood spiral: less activity → more stiffness → worse pain → lower mood → even less activity. The good news is that breaking this loop doesn’t require expensive interventions — just structure, awareness, and consistency.
When using meloxicam or any anti-inflammatory, it helps to treat medication as a tool for movement, not just symptom relief. Plan to take the dose around times when you can move safely: morning stretching, household tasks, or short walks. These small, purposeful movements reinforce confidence and keep joints lubricated. Think of them as “green-zone” tasks: light activities that build tolerance without flare-ups. Instead of waiting for zero pain before resuming activity, aim for micro-movement: gentle, frequent motion in 10–15 minute bursts spaced through the day. Even low-intensity tasks like watering plants, tidying a desk, standing to stretch, maintain circulation and endorphin flow. The body reads these as safety signals, gradually calming pain sensitivity.
This approach mirrors principles of behavioral activation, a therapy originally designed for depression. Scheduling small, rewarding actions reduces emotional inertia, improves mood, and indirectly decreases pain perception. Physical improvement then reinforces optimism — a feedback loop in the right direction.
Meloxicam can play a supportive role here by blunting enough inflammation to make these micro-steps possible. But medication alone cannot restore function; movement plus mindset completes the process. Pair NSAID use with realistic activity goals: “I’ll walk for five minutes,” not “I’ll walk pain-free.” Over time, confidence replaces fear as the primary driver.
To stay accountable, keep a pain–function diary noting activity type, duration, and next-day effect. This reframes success from pain elimination to mobility gained — a more sustainable metric.
Finally, set a quit rule: if there’s no measurable functional improvement after 7–10 days, or if new red flags appear (swelling, fatigue, GI symptoms), pause the medication and reassess with your clinician. Overstaying on an ineffective regimen wastes both health and money.
The most cost-effective pain plan isn’t about the cheapest drug, it’s about using affordable medication to re-enable affordable motion. Function, not complete comfort, should be the benchmark of success.
Conclusion
Meloxicam combines affordability with effectiveness, but its real value lies in how it’s used. When taken thoughtfully, at the lowest effective dose, for a clear duration, and alongside movement-based recovery, it can relieve pain without compromising long-term safety. The aim is not to chase total absence of pain but to restore function, flexibility, and confidence.
Medication alone rarely solves chronic discomfort. Pairing meloxicam with activity pacing, healthy routines, and self-awareness keeps both pain and mood in balance. If relief plateaus or side effects emerge, a brief pause and reassessment protect against harm and wasted effort.
Used wisely, meloxicam is more than a budget-friendly painkiller, it’s a bridge back to motion and participation in daily life.
